Search
- Page Path
- HOME > Search
Original Article
- Impact of anterior chamber depth to axial length ratio on conventional intraocular lens power calculation formulas performance in axial myopia
- Youngsub Eom, Jinhwan Park, Youngbin Song, Dong Hyun Kim, Jong Suk Song
- Insights Cataract Refract Surg 2026;11(1):15-22. Published online February 26, 2026
- DOI: https://doi.org/10.63375/icrs.25.017

-
 Abstract
Abstract
 PDF
PDF ePub
ePub - Purpose
To evaluate the effects of the ratio of anterior chamber depth to axial length (ACD/AL), as well as axial length (AL) itself, on the accuracy of conventional intraocular lens (IOL) power calculation formulas in eyes with axial myopia.
Methods
This retrospective cross-sectional study included 60 eyes from 44 patients with an AL greater than 25.0 mm who underwent uncomplicated phacoemulsification with IOL implantation. Eyes were categorized into high and low AL groups using an AL threshold of 27.0 mm, and into high and low ACD/AL groups based on the median ACD/AL value of 13.4. The median absolute errors (MedAEs) predicted by the Sanders-Retzlaff-Kraff theoretical (SRK/T) and Haigis formulas were compared according to AL and ACD/AL groupings.
Results
In the low ACD/AL group and in the high AL group, the MedAEs predicted by the Haigis formula were lower than those predicted by the SRK/T formula (P=0.002 and P=0.012, respectively). The MedAEs predicted by both the SRK/T and Haigis formulas were significantly lower in the high ACD/AL group than in the low ACD/AL group (P<0.001 and P=0.010, respectively). In contrast, no significant difference was observed between the low and high AL groups in the MedAEs predicted by the Haigis formula. When the ACD/AL ratio was less than 13.4, postoperative refractive outcomes were more hyperopic with both formulas.
Conclusion
In eyes with a long AL and a relatively shallow ACD, the Haigis formula demonstrated superior accuracy among conventional IOL power calculation formulas. Under these anatomical conditions, targeting slightly more myopic postoperative refractions may therefore be advisable.
- 310 View
- 5 Download

Review Article
- Presbyopia-correcting intraocular lens options in myopic eyes undergoing cataract surgery
- Sang Beom Han
- Insights Cataract Refract Surg 2026;11(1):1-8. Published online February 26, 2026
- DOI: https://doi.org/10.63375/icrs.25.016
-
 Abstract
Abstract
 PDF
PDF ePub
ePub - With ongoing advancements in surgical techniques and intraocular lens (IOLs) technologies, cataract surgery is increasingly recognized as a form of refractive procedure aimed at enhancing overall visual performance rather than being viewed solely as lens extraction. In parallel with this shift, a growing number of aging individuals with myopia are actively seeking spectacle independence following cataract surgery. The selection of IOLs for presbyopia correction in patients with myopia presents distinct clinical and refractive challenges, necessitating careful preoperative evaluation and individualized surgical planning. In this review, the author summarizes current evidence regarding the use of various IOLs, including monofocal, enhanced monofocal, extended depth-of-focus, and multifocal IOLs, for presbyopia correction in myopic patients and discusses key considerations involved in selecting the most appropriate IOL for this specific population.
- 288 View
- 4 Download

Original Article
- Visual and refractive outcomes of keratorefractive lenticule extraction using VISUMAX 800 (SMILE Pro) to correct myopia in Koreans: a 3-month follow-up study
- Sang-Mok Lee, Si-Hoon Park, Tae Keun Yoo, Jae Hyoung Park, Beom Jin Cho, Kee Yong Choi, Jong Woo Kim
- Insights Cataract Refract Surg 2025;10(1):13-18. Published online February 28, 2025
- DOI: https://doi.org/10.63375/icrs.25.004
-
 Abstract
Abstract
 PDF
PDF ePub
ePub - Purpose
The aim of this study was to report the clinical outcomes of SMILE Pro surgery in Korean myopia patients.
Methods
A retrospective analysis was conducted on the medical records of 90 patients (178 eyes) who underwent SMILE Pro surgery at our institution between October 2023 and June 2024 and were followed for 3 months postoperatively.
Results
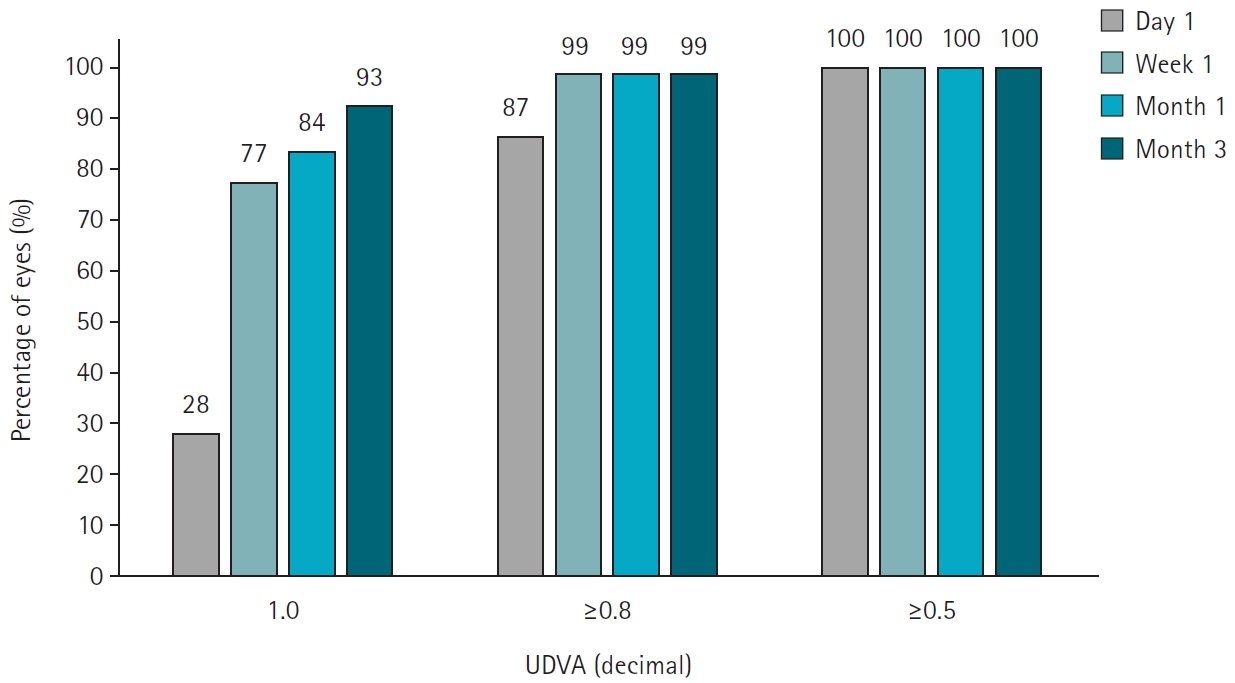
Preoperative best corrected visual acuity was 0.009±0.020 (logarithm of the minimum angle of resolution). The average spherical equivalent was –5.13±2.16 diopters (range, –1.00 to –10.10 diopters), and the average astigmatism was –1.21±0.91 diopters (range, 0 to –4.0 diopters). Postoperatively, the uncorrected distance visual acuity at 1 day, 1 week, 1 month, and 3 months were 0.061±0.054, 0.013±0.027, 0.009±0.023, 0.005±0.021, respectively. At 3 months postsurgery, the predictive accuracy for spherical equivalent was 100% within ±0.5 diopters and 98.9% within ±0.25 diopters. For astigmatism, the predictive accuracy was 97.2% within ±0.25 diopters and 99.4% within ±0.5 diopters 97.2% and 99.4%. The scores for the efficacy and safety of refractive surgery at 3 months were both 1.01±0.05.
Conclusion
SMILE Pro surgery for myopia correction in Korean patients demonstrated excellent efficacy, safety, and predictive accuracy, with no significant difference compared to conventional SMILE surgery.
- 1,757 View
- 24 Download


 KSCRS
KSCRS
 First
First Prev
Prev