Funded articles
- Page Path
- HOME > Browse articles > Funded articles
Case Report
- Large incisional tear caused by abrupt Bell’s phenomenon during pocket irrigation in femtosecond laser-assisted small incision lenticule extraction
- Sang Beom Han
- Insights Cataract Refract Surg 2026;11(1):23-25. Published online February 26, 2026
- DOI: https://doi.org/10.63375/icrs.25.015
- Funded: National Research Foundation of Korea, Ministry of Education

-
 Abstract
Abstract
 PDF
PDF ePub
ePub - Purpose
This study reports a case of a large incisional tear caused by abrupt Bell’s phenomenon during pocket irrigation in femtosecond laser-assisted small incision lenticule extraction (SMILE).
Case
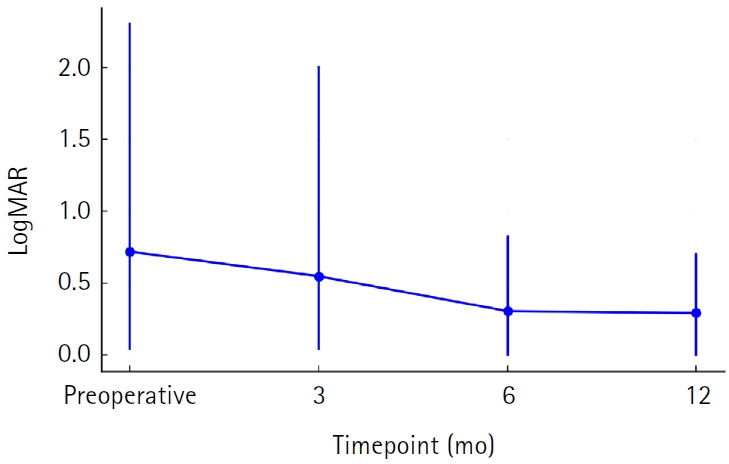
summary: A 28-year-old male patient underwent SMILE surgery. During pocket irrigation of the right eye, Bell’s phenomenon suddenly occurred, resulting in a large inferior arcuate extension of the incision that reached the inferior cap margin. After confirming wound integrity and the absence of additional tissue damage, a bandage contact lens was applied. On postoperative day 7, the incision was self-sealed with intact wound integrity. Three months postoperatively, uncorrected distance visual acuity was 20/20 in both eyes. The right cornea remained stable, although a faint residual scar was observed at the site of the incisional tear.
Conclusion
Abrupt eye movements during pocket irrigation in SMILE can cause large incisional tears. Surgeons should exercise heightened vigilance during irrigation, particularly in anxious or uncooperative patients, to prevent such complications.
- 228 View
- 2 Download

Original Article
- Therapeutic effects of diquafosol ophthalmic solution and carbomer eye gel in dry eye patients with lid wiper epitheliopathy
- Jong Suk Song, In Ho Woo
- Insights Cataract Refract Surg 2026;11(1):9-14. Published online February 26, 2026
- DOI: https://doi.org/10.63375/icrs.25.019
- Funded: National Research Foundation of Korea, Ministry of Education

-
 Abstract
Abstract
 PDF
PDF ePub
ePub - Purpose
This study aimed to evaluate the therapeutic effects of 3% diquafosol tetrasodium ophthalmic solution (Diquas) and a carbomer-based, lipid-containing eye gel (Liposic, Bausch & Lomb) in dry eye patients with lid wiper epitheliopathy (LWE) that was refractory to topical treatment with conventional artificial tears.
Methods
Thirty-three dry eye patients with LWE of the upper eyelid were treated with 3% diquafosol ophthalmic solution administered six times daily and a carbomer-based, lipid-containing eye gel administered four times daily. After the 2-week treatment period, changes in ocular symptoms were assessed using a visual analog scale (VAS), and changes in ocular signs were evaluated using tear film break-up time (TBUT), corneal staining, and LWE grading.
Results
The mean patient age was 37.58±12.35 years (range, 21–67 years); six patients were male and 27 were female. At baseline, the mean VAS symptom score was 7.18±1.47, and the mean TBUT was 2.78±0.78 seconds. After 2 weeks of treatment, the mean VAS score decreased to 4.87±1.97, and the mean TBUT increased to 3.68±1.08 seconds (both P<0.05). The mean corneal staining score was 1.09±1.50, and the mean LWE grade was 5.76±0.61 at baseline. Following treatment, these values decreased to 0.55±0.83 and 2.24±1.95, respectively (both P<0.05). Among the objective parameters, only the LWE grade showed a significant correlation with the VAS score.
Conclusion
The LWE grade showed a significant correlation with ocular symptoms. Combined treatment with diquafosol ophthalmic solution and a carbomer-based, lipid-containing eye gel demonstrated excellent therapeutic effects in dry eye patients with LWE who were refractory to treatment with conventional artificial tears.
- 407 View
- 7 Download

Review Article
- Presbyopia-correcting intraocular lens options in myopic eyes undergoing cataract surgery
- Sang Beom Han
- Insights Cataract Refract Surg 2026;11(1):1-8. Published online February 26, 2026
- DOI: https://doi.org/10.63375/icrs.25.016
- Funded: National Research Foundation of Korea, Ministry of Education
-
 Abstract
Abstract
 PDF
PDF ePub
ePub - With ongoing advancements in surgical techniques and intraocular lens (IOLs) technologies, cataract surgery is increasingly recognized as a form of refractive procedure aimed at enhancing overall visual performance rather than being viewed solely as lens extraction. In parallel with this shift, a growing number of aging individuals with myopia are actively seeking spectacle independence following cataract surgery. The selection of IOLs for presbyopia correction in patients with myopia presents distinct clinical and refractive challenges, necessitating careful preoperative evaluation and individualized surgical planning. In this review, the author summarizes current evidence regarding the use of various IOLs, including monofocal, enhanced monofocal, extended depth-of-focus, and multifocal IOLs, for presbyopia correction in myopic patients and discusses key considerations involved in selecting the most appropriate IOL for this specific population.
- 288 View
- 4 Download

Original Article
- Clinical results of combined Descemet membrane keratoplasty and cataract operation (triple Descemet membrane keratoplasty) from imported donor corneas: a retrospective study
- Hyung Keun Lee, Sung Soo Kang, Jin Suk Chun, So Young Kim, Dong Ihll Lee
- Insights Cataract Refract Surg 2025;10(3):83-90. Published online October 31, 2025
- DOI: https://doi.org/10.63375/icrs.25.014
- Funded: National Research Foundation of Korea, Ministry of Education, Science, and Technology
-
 Abstract
Abstract
 PDF
PDF ePub
ePub - Purpose
This study reports the clinical outcomes, after triple Descemet membrane endothelial keratoplasty (DMEK) performed using imported corneas.
Methods
A retrospective study was conducted on 30 eyes of 26 patients who underwent Descemet's membrane keratoplasty concurrently with cataract surgery, referred to as triple DMEK, from January 2023 to June 2025. After routine preoperative examinations for keratoplasty as well as cataract surgery, uneventful DMEK surgery was performed concurrently with cataract surgery. All patients visited the clinic at 1, 3, 6, and 12 months after surgery to observe changes, including uncorrected and best spectacle corrected visual acuity, refractive error, corneal thickness, and endothelial cell density.
Results
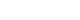
Preoperatively, 12 of the 30 eyes had Fuchs corneal endothelial dystrophy and 12 had endothelial failure following phakic intraocular lens implantation. The average observation period for the subjects was 437±263 days. After triple DMEK surgery, the patients' uncorrected visual acuity gradually improved from 0.73±0.6 (logMAR) before surgery to 0.65±0.54 at 3 months and 0.29±0.26 at 1 year (P<0.001). The change in corneal thickness was 565.7±70.0 μm before surgery, 535.2±44.2 μm at 3 months after surgery, 549.7±73.5 μm at 6 months, and 535.82±49.0 μm at 12 months, but no statistical significance was found compared to before surgery at any time point (P>0.05). The endothelial cell density was 798±363 cells/mm2 before surgery, 1,479±475 cells/mm2 at 3 months after surgery, 1,456±456 cells/mm2 at 6 months, 1,332±346 cells/mm2 at 12 months, and 1,399±519 cells/mm2 at the last visit (P<0.001).
Conclusion
Triple DMEK surgery, which is performed for various corneal diseases, is relatively safe. No significant endothelial damage, refractive changes, or visual acuity abnormalities were observed up to one year after surgery. Future prospective studies including a larger number of participants are warranted to evaluate the safety and clinical outcomes of triple DMEK using imported corneas.
- 618 View
- 6 Download

Case Report
- Diffuse lamellar keratitis after small incision lenticule extraction: presumably related to meibomian gland dysfunction
- Sang Beom Han
- Insights Cataract Refract Surg 2025;10(2):61-64. Published online June 30, 2025
- DOI: https://doi.org/10.63375/icrs.25.008
- Funded: National Research Foundation of Korea, Ministry of Education
-
 Abstract
Abstract
 PDF
PDF ePub
ePub - Purpose
This report presents a case of diffuse lamellar keratitis (DLK) after femtosecond laser-assisted small incision lenticule extraction (SMILE). The case was presumably associated with meibomian gland dysfunction (MGD).
Case
summary: A 25-year-old male patient underwent SMILE surgery. Preoperative examination revealed MGD in both eyes. Despite vigorous cleaning of the eyelid margin and irrigation of the ocular surface, meibomian gland secretion floating on the ocular surface was observed after the lenticule extraction in the right eye. At 2 days postoperatively, stage I DLK was detected. After aggressive topical steroid treatment, the DLK completely resolved without any sequalae.
Conclusion
DLK can occur in association with MGD. Attention should be paid when performing SMILE in eyes with MGD.
- 2,814 View
- 21 Download

Review Article
- Selection of an optimal intraocular lens according to the stage of epiretinal membrane
- Sang Beom Han
- Insights Cataract Refract Surg 2025;10(1):7-12. Published online February 28, 2025
- DOI: https://doi.org/10.63375/icrs.25.003
- Funded: National Research Foundation of Korea, Ministry of Education
-
 Abstract
Abstract
 PDF
PDF ePub
ePub - Epiretinal membrane (ERM), one of the most common retinal diseases, can cause various degrees of visual disturbance, reduced contrast sensitivity, and metamorphopsia. ERM is not infrequently encountered during preoperative evaluations for cataract surgery, and selecting an appropriate intraocular lens (IOL) according to the location and stage of ERM is necessary in order to improve visual outcomes and patients’ satisfaction. This review summarizes the application of various IOLs—such as multifocal, extended depth of focus, and enhanced monofocal IOLs—in eyes with ERM, and discusses the selection of an appropriate IOL.
-
Citations
Citations to this article as recorded by- Presbyopia-correcting intraocular lens options in myopic eyes undergoing cataract surgery
Sang Beom Han
Insights in Cataract and Refractive Surgery.2026; 11(1): 1. CrossRef
- Presbyopia-correcting intraocular lens options in myopic eyes undergoing cataract surgery
- 1,285 View
- 19 Download
- 1 Crossref


 KSCRS
KSCRS

 First
First Prev
Prev