Abstract
-
Purpose
- This study aimed to evaluate the therapeutic effects of 3% diquafosol tetrasodium ophthalmic solution (Diquas) and a carbomer-based, lipid-containing eye gel (Liposic, Bausch & Lomb) in dry eye patients with lid wiper epitheliopathy (LWE) that was refractory to topical treatment with conventional artificial tears.
-
Methods
- Thirty-three dry eye patients with LWE of the upper eyelid were treated with 3% diquafosol ophthalmic solution administered six times daily and a carbomer-based, lipid-containing eye gel administered four times daily. After the 2-week treatment period, changes in ocular symptoms were assessed using a visual analog scale (VAS), and changes in ocular signs were evaluated using tear film break-up time (TBUT), corneal staining, and LWE grading.
-
Results
- The mean patient age was 37.58±12.35 years (range, 21–67 years); six patients were male and 27 were female. At baseline, the mean VAS symptom score was 7.18±1.47, and the mean TBUT was 2.78±0.78 seconds. After 2 weeks of treatment, the mean VAS score decreased to 4.87±1.97, and the mean TBUT increased to 3.68±1.08 seconds (both P<0.05). The mean corneal staining score was 1.09±1.50, and the mean LWE grade was 5.76±0.61 at baseline. Following treatment, these values decreased to 0.55±0.83 and 2.24±1.95, respectively (both P<0.05). Among the objective parameters, only the LWE grade showed a significant correlation with the VAS score.
-
Conclusion
- The LWE grade showed a significant correlation with ocular symptoms. Combined treatment with diquafosol ophthalmic solution and a carbomer-based, lipid-containing eye gel demonstrated excellent therapeutic effects in dry eye patients with LWE who were refractory to treatment with conventional artificial tears.
-
Keywords: Lid wiper epitheliopathy; Friction; Blinking; Mucin secretagogue
Introduction
According to Korb et al. [1,2], the anatomical area of the lid wiper region is the portion of the palpebral marginal conjunctiva in the upper and lower lids that is in contact with the ocular globe. In the upper lid, it extends from the crest of the sharp posterior (inner) lid border (i.e., the mucocutaneous junction or line of Marx) to the subtarsal fold vertically and from the medial upper punctum to the lateral canthus horizontally.
Lid wiper epitheliopathy (LWE) is a clinically observable alteration in the epithelium of the lid wiper area, the portion of the marginal conjunctival epithelium of the upper eyelid that wipes the ocular surface during blinking [3,4]. The tear film is composed of a mixture of lipids, lacrimal fluid, and mucins [5]. In patients with dry eye, the tear film is thought to be insufficient to lubricate the friction between the ocular surface and the lid wiper. Due to the increased friction, the lid wiper area is subjected to trauma during blinking as a result of continual rubbing of the narrow surface area of lid wiper tissue against the corneal surface [3,6]. LWE may be caused by mechanical forces during blinking, resulting in inflammation of the ocular surface [7].
The incidence of LWE is higher in patients having both dry eye symptoms and signs compared with normal control patients who have no symptoms and signs [8]. However, LWE was reported to occur in subjects with dry eye symptoms despite the absence of positive dry eye test findings, providing a potential answer to the portion of the spectrum of dry eye disease in which signs and symptoms did not correlate well [2].
Therefore, the purpose of this study was to investigate the associations between LWE and other parameters of dry eye disease and to determine the effectiveness of combined therapy of 3% diquafosol ophthalmic solution (Diquas, Santen) as a mucin secretagogue and a carbomer-based, lipid-containing eye gel (Liposic, Bausch & Lomb) to reduce the friction between the lid wiper area and the ocular surface.
Methods
Ethics statement
This study followed the tenets of the Declaration of Helsinki. This study was approved by the Institutional Review Board of Korea University Guro Hospital.
Patient and study design
We retrospectively reviewed patients who were diagnosed with LWE associated with dry eye disease at the Department of Ophthalmology of Korea University Guro Hospital, from February to June of 2017. A total of 33 eyes in 33 patients with LWE who were refractory to topical medication with conventional artificial tears.
Thirty-three dry eye patients with LWE of the upper eyelid were treated with 3% diquafosol ophthalmic solution six times a day and a carbomer-based, lipid-containing eye gel four times a day were enrolled in this study.
All patients were diagnosed with dry eye disease according to the Dry Eye Workshop Ⅱ guidelines [9]. All patients were treated using a 3% diquafosol ophthalmic solution and carbomer-based, lipid-containing eye gel. The exclusion criteria were systemic disease that might affect the tear film, a history of ocular trauma or ocular surgery, bacterial or viral infection of the cornea and conjunctiva, and use of contact lenses for 3 months. The eye with a higher LWE grade was selected from each patient. When the LWE grade was the same in both eyes, the eye with the higher corneal staining score was selected.
Clinical measurements
Subjective dry eye symptoms were evaluated using a visual analog scale (VAS) from 0 to 10 points. Patients described their ocular pain and discomfort intensity due to dry eye disease. If there was no pain and discomfort, the score was 0 points, and if there was very severe pain or discomfort, the score was 10 points. Objective assessments were evaluated for LWE, tear film break-up time (TBUT), and fluorescein corneal staining score. After instillation of fluorescein dye, the ocular surface was examined under the combination of a yellow filter and the highest cobalt blue illumination using a slit-lamp (Haag-Streit 900, Haag Streit) [10]. In accordance with the National Eye Institute (NEI) classification, the cornea was divided into five areas, with each area assigned a maximum staining score of 3 points, resulting in a total maximum score of 15 points.
LWE was graded from 0 to 6 points using a modified Korb’s grading system [1-4]. The stained horizontal length and sagittal width were separately graded from 0 to 3 points, and the final grade was determined as the sum of stained horizontal length and sagittal width. The corneal fluorescein staining score was graded from 0 to 15 points using the NEI scoring scheme [6]. After contacting the conjunctival sac with fluorescent staining paper, the eyes were blinked more than three times for several seconds to uniformly apply the dye to the surface of the cornea, and then the TBUT test was performed. TBUT, the interval between blinking and the first appearance of a dry spot on the tear film, was measured three times, and the mean value of the three measurements was used.
Treatment protocol
The protocol to treat dry eye patients with LWE was 3% diquafosol ophthalmic solution six times a day and a carbomer-based, lipid-containing eye gel four times a day. Diquafosol has been reported to increase tear film stability and improve symptoms related to dry eye disease [11-14]. Carbomer-based, lipid-containing eye gel (Liposic Gel, Bausch & Lomb), contains 94% water, 0.2% carbomer, and 1% medium-chain triglyceride. These carbomer-based, lipid-containing gels have been reported to improve symptoms and signs associated with dry eye disease [15-17]. To minimize friction between the eyelid and the ocular surface, the two topical medications were used together to treat patients with LWE for 2 weeks.
Statistical analyses
Statistical analyses were performed using the IBM SPSS ver. 21.0 (IBM Corp.). All data are presented as mean±standard deviation. Paired t-test was used to compare changes in variables before and after treatment. Correlations among subjective symptoms and objective parameters were evaluated by Pearson correlation analysis. A P-value less than 0.05 was considered statistically significant.
Results
A total of 33 patients was included in this study. Their mean age was 37.58±12.35 years. Of these patients, six were male and 27 were female (81.8%). Table 1 summarizes the mean±standard deviation of grade of LWE, VAS score, corneal staining score, and TBUT.
After the 2-week treatment, the VAS symptom score significantly decreased from 7.18±1.47 to 4.87±1.97 (P<0.001). The corneal staining score based on NEI scheme significantly decreased from 1.09±1.50 to 0.55±0.83 (P=0.024), and TBUT significantly increased from 2.78±0.78 to 3.68±1.08 seconds after the 2-week treatment (P<0.001) (Table 2). After the 2-week treatment, the horizontal length grade of LWE decreased from 2.97±0.17 to 1.48±1.37, and the sagittal width grade decreased from 2.79±0.54 to 0.76±0.66. The LWE, the sum of the two states, significantly decreased from 5.76±0.61 to 2.24±1.95 (Figs. 1, 2).
In the correlation analysis between dry eye parameters at baseline, age positively correlated with corneal staining score and negatively correlated with TBUT. The corneal staining score negatively correlated with TBUT. However, VAS symptom score only correlated with grade of LWE (r=0.482) (Table 3). Even after the 2-week treatment, VAS symptom score showed significant correlation only with the grade of LWE (Table 4).
Discussion
The term LWE was first used by Korb et al. [1,2]. This occurrence was detected by ocular staining with alteration of the marginal conjunctival epithelium of the upper eyelid that wipes the ocular surface during blinking. LWE, which is related to the mechanical force generated during eye blinking, eventually leads to irritation of the ocular surface. Korb et al. [2] reported the relationship between LWE and dry eye syndrome and found that the degree of LWE was high when dry eye symptoms were severe. This was due to instability of the tear film, increase in friction between lid wiper area and bulbar conjunctiva, and decrease in mucin secretion [7]. Yeniad et al. [18] evaluated LWE in contact lens users, symptomatic dry eye patients, and normal controls. They found that the prevalence of LWE was higher in contact lens wearers with ocular discomfort symptoms than in contact lens wearers without ocular discomfort. In addition, dry eye patients had a higher prevalence of LWE than the control group. However, there was no correlation between LWE and TBUT.
In this study, the mean LWE grade was 5.76±0.61 out of 6, and the mean VAS score, which was a measurement of ocular discomfort from 0 to 10 points, was 7.18±1.47. However, the mean corneal staining score was 1.09±1.50, which was relatively lower compared with the mean symptom score. The mean TBUT was 2.78±0.78 seconds. The subjects in this study showed minimal corneal staining score, short TBUT, high LWE grade, and severe symptom score. Although there was no correlation between LWE and TBUT, grade of LWE was the only parameter that significantly correlated with ocular discomfort symptom (VAS) score. This correlation was found in baseline examination and after the 2-week treatment.
In normal eyes, tears are constantly secreted and cover the ocular surface. The tear film is composed of a lipid layer and an aqueous-mucous layer [5]. Mucins play an important role in tear film stability and protecting the ocular surface. These mucins are classified as secretory mucins and membrane-associated mucins [19,20]. Diquafosol tetrasodium acts as a P2Y2 receptor agonist to promote tear secretion from conjunctival epithelium and mucin secretion from conjunctival goblet cells [12-15]. In previous studies, diquafosol stimulated MUC5A secretion from conjunctival goblet cells and increased membrane-associated mucins, such as MUC1, MUC4, and MUC16, in corneal epithelial cells [21,22]. Diquafosol tetrasodium is now commonly used as a mucin secretagogue to treat dry eye patients in many Asian countries.
LWE is caused by frictional forces between the ocular surface and the upper eyelid during blinking. Several studies have examined the change of LWE after using lubricating eye drops to solve this problem. Guthrie et al. [23] reported that the propylene glycol-based Systane Balance lubricant eye drop was effective in early treatment of LWE and long-term improvement of the lid wiper epithelium. Ngo et al. [24] investigated the therapeutic effects of the TheraTears nutrition formulation containing sodium carboxymethyl cellulose and reported that ocular discomfort, non-invasive tear break-up time, and meibomian gland function improved, but that there was no significant difference in LWE. Itakura et al. [25] reported the therapeutic effects of rebamipid on LWE. Similarly, rebamipid also increased the secretion of both secretory and membrane-associated mucins in conjunctival goblet cells and corneal epithelial cells. The authors suggested that rebamipid was effective in treating patients with LWE. However, it was difficult to determine the statistical significance or therapeutic effect because only two cases were analyzed. In our study, we evaluated 33 patients with LWE and confirmed the therapeutic effects of diquafosol on LWE. Liposic Gel, containing the carbomer component, was used together with diquafosol in our study. Therefore, it was difficult to confirm the therapeutic effects of Liposic Gel and diquafosol solution separately. However, both topical medications were used to achieve maximal therapeutic effects to reduce friction, and even after the 2 weeks of short-term treatment, a significant improvement was found in LWE grade.
To date, various eye drops and treatments have been proposed as therapeutic agents for LWE [26]. However, there has been no study on the combined treatment of these two agents. Therefore, this study is of great significance for the efficacy of combined therapy using mucin secretagogue and carbomer lubrication gel as a treatment modality for LWE. After two weeks of short-term administration to the study subjects, various parameters of dry eye disease improved, including LWE grade, corneal staining score, TBUT, and VAS symptom score.
In conclusion, grade of LWE was the only parameter that significantly correlated with ocular discomfort symptom (VAS) score. The combined therapy using diquafosol ophthalmic solution and carbomer eye gel even after a short, 2-week treatment showed excellent therapeutic effects on dry eye patients with LWE who were refractory to topical medication with conventional artificial tears.
Article Information
Author contributions
Conceptualization: JSS. Formal analysis: JSS. Investigation: JSS. Methodology: IHW. Supervision: JSS. Writing - original draft: IHW. Writing - review & editing: JSS. Final approval of the manuscript: all authors.
Conflicts of interest
No potential conflict of interest relevant to this article was reported.
Funding
This research was supported by the Basic Science Research Program through the National Research Foundation of Korea (NRF) and funded by the Ministry of Education (NRF-2017R1D1A1B03028552). The funding organization had no role in the design or conduct of this research.
Data availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
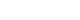
Fig. 1.A 35-year-old female patient. Slit-lamp examination performed using a yellow filter and maximal cobalt blue illumination with fluorescein staining demonstrated lid wiper staining (A) and a clear corneal state (B). After 2 weeks of topical treatment with Diquas and Liposic, lid wiper staining was markedly improved (C), and the corneal state remained clear (D).
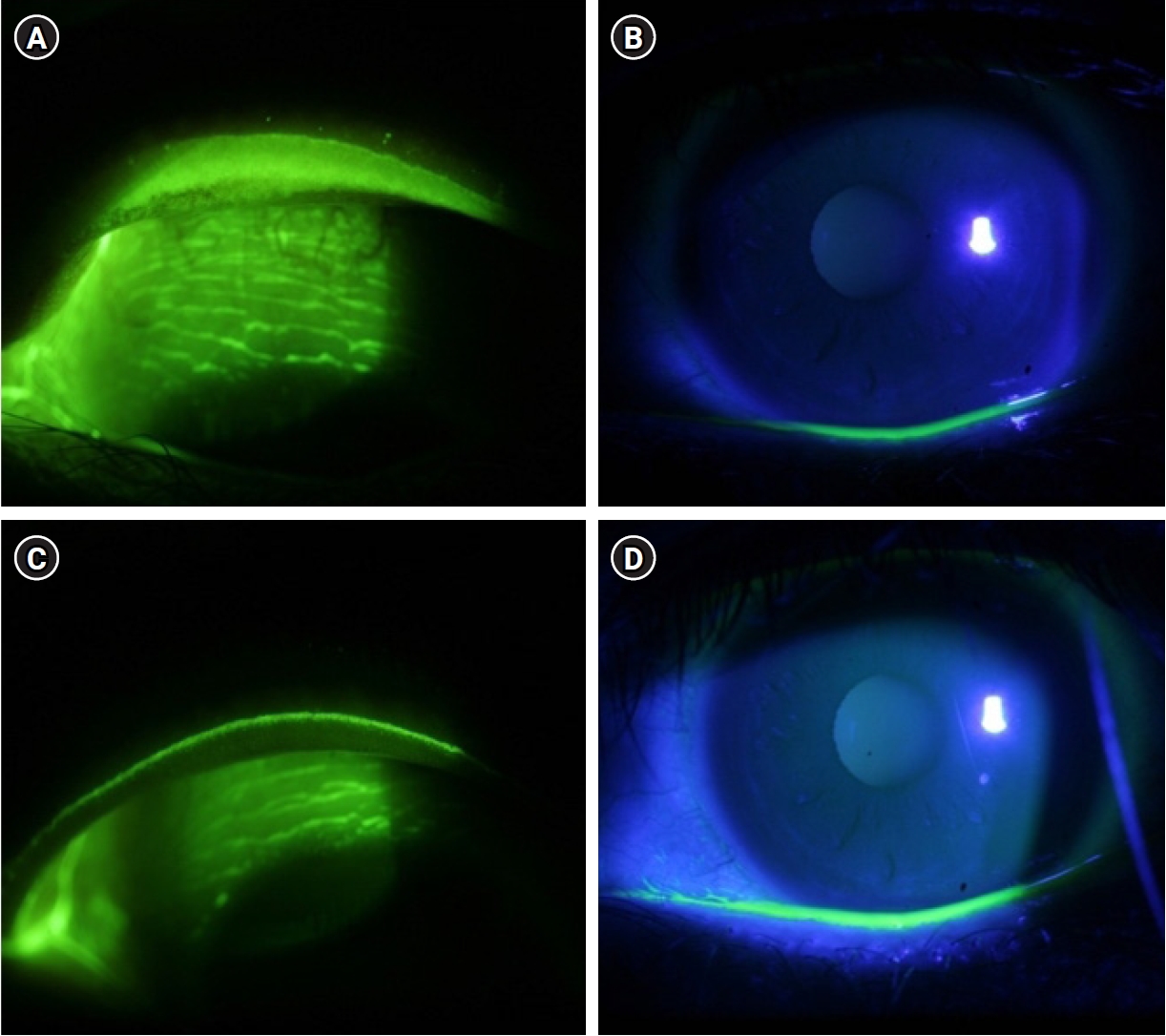
Fig. 2.Graphs illustrating lid wiper epitheliopathy (LWE) grade before and after treatment.
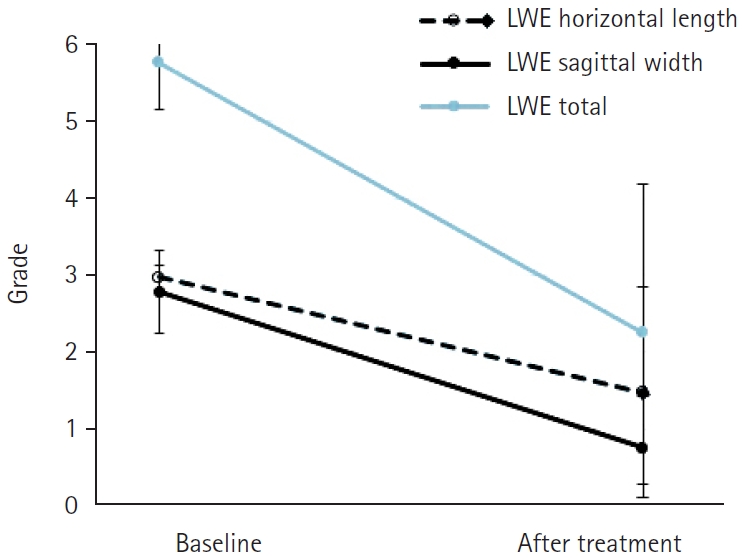
Table 1.Patient demographics
|
Characteristic |
Value |
|
Age (yr) |
37.58±12.35 |
|
Sex (male:female) |
6:27 |
|
Lid wiper epitheliopathy (grade) |
|
|
Horizontal length |
2.97±0.17 |
|
Sagittal width |
2.79±0.54 |
|
Total |
5.76±0.61 |
|
Visual analog scale (score) |
7.18±1.47 |
|
Corneal staining (score) |
1.09±1.50 |
|
Tear film break-up time (sec) |
2.78±0.78 |
|
|
Table 2.Changes in dry eye parameters after treatment
|
Parameter |
Baseline |
After treatment |
P-value |
|
Lid wiper epitheliopathy |
|
|
|
|
Horizontal length |
2.97±0.17 |
1.48±1.37 |
<0.001 |
|
Sagittal width |
2.79±0.54 |
0.76±0.66 |
<0.001 |
|
Total |
5.76±0.61 |
2.24±1.95 |
<0.001 |
|
Visual analog scale (score) |
7.18±1.47 |
4.87±1.97 |
<0.001 |
|
Corneal staining (score) |
1.09±1.50 |
0.55±0.83 |
0.024 |
|
Tear film break-up time (sec) |
2.78±0.78 |
3.68±1.08 |
<0.001 |
Table 3.Correlations between parameters before treatment
|
Parameter |
Age |
LWE |
VAS |
Corneal staining |
TBUT |
|
Age |
- |
|
|
|
|
|
LWE |
0.159 |
- |
|
|
|
|
VAS |
–0.143 |
0.482*
|
- |
|
|
|
Corneal staining |
0.395*
|
0.126 |
0.105 |
- |
|
|
TBUT |
–0.460*
|
–0.241 |
–0.183 |
–0.408*
|
- |
Table 4.Correlations between parameters after treatment
|
Parameter |
Age |
LWE |
VAS |
Corneal staining |
TBUT |
|
Age |
- |
|
|
|
|
|
LWE |
–0.099 |
- |
|
|
|
|
VAS |
–0.047 |
0.364*
|
- |
|
|
|
Corneal staining |
0.090 |
0.301 |
0.117 |
- |
|
|
TBUT |
–0.050 |
–0.337 |
–0.251 |
–0.389*
|
- |
References
- 1. Korb DR, Greiner JV, Herman JP, et al. Lid-wiper epitheliopathy and dry-eye symptoms in contact lens wearers. CLAO J 2002;28:211‒6. ArticlePubMed
- 2. Korb DR, Herman JP, Greiner JV, et al. Lid wiper epitheliopathy and dry eye symptoms. Eye Contact Lens 2005;31:2‒8. ArticlePubMed
- 3. Korb DR, Herman JP, Finnemore VM, et al. An evaluation of the efficacy of fluorescein, rose bengal, lissamine green, and a new dye mixture for ocular surface staining. Eye Contact Lens 2008;34:61‒4. ArticlePubMed
- 4. Korb DR, Herman JP, Blackie CA, et al. Prevalence of lid wiper epitheliopathy in subjects with dry eye signs and symptoms. Cornea 2010;29:377‒83. ArticlePubMed
- 5. Willcox MD, Argueso P, Georgiev GA, et al. TfOS DEWS II tear film report. Ocul Surf 2017;15:366‒403. ArticlePubMedPMC
- 6. Yamamoto Y, Shiraishi A, Sakane Y, et al. Involvement of eyelid pressure in lid-wiper epitheliopathy. Curr Eye Res 2016;41:171‒8. ArticlePubMed
- 7. Berry M, Pult H, Purslow C, Murphy PJ. Mucins and ocular signs in symptomatic and asymptomatic contact lens wear. Optom Vis Sci 2008;85:E930‒8. ArticlePubMed
- 8. Pult H, Purslow C, Murphy PJ. The relationship between clinical signs and dry eye symptoms. Eye (Lond) 2011;25:502‒10. ArticlePubMedPMCPDF
- 9. Wolffsohn JS, Arita R, Chalmers R, et al. TfOS DEWS II diagnostic methodology report. Ocul Surf 2017;15:539‒74. ArticlePubMed
- 10. Eom Y, Lee JS, Lee HK, et al. Comparison of conjunctival staining between lissamine green and yellow filtered fluorescein sodium. Can J Ophthalmol 2015;50:273‒7. ArticlePubMed
- 11. Lemp MA. Report of the National Eye Institute/Industry workshop on clinical trials in dry eyes. CLAO J 1995;21:221‒32. PubMed
- 12. Fujihara T, Murakami T, Nagano T, et al. INS365 suppresses loss of corneal epithelial integrity by secretion of mucin-like glycoprotein in a rabbit short-term dry eye model. J Ocul Pharmacol Ther 2002;18:363‒70. ArticlePubMed
- 13. Matsumoto Y, Ohashi Y, Watanabe H, Tsubota K. Efficacy and safety of diquafosol ophthalmic solution in patients with dry eye syndrome: a Japanese phase 2 clinical trial. Ophthalmology 2012;119:1954‒60. ArticlePubMed
- 14. Tauber J, Davitt WF, Bokosky JE, et al. Double-masked, placebo-controlled safety and efficacy trial of diquafosol tetrasodium (INS365) ophthalmic solution for the treatment of dry eye. Cornea 2004;23:784‒92. ArticlePubMed
- 15. Nakamura M, Imanaka T, Sakamoto A. Diquafosol ophthalmic solution for dry eye treatment. Adv Ther 2012;29:579‒89. ArticlePDF
- 16. Marner K, Mooller PM, Dillon M, Rask-Pedersen E. Viscous carbomer eye drops in patients with dry eyes: efficacy and safety: a randomized, open, cross-over, multicentre study. Acta Ophthalmol Scand 1996;74:249‒52. PubMed
- 17. Chung SH, Lim SA, Tchach H. Efficacy and safety of carbomer-based lipid-containing artificial tear formulations in patients with dry eye syndrome. Cornea 2016;35:181‒6. ArticlePubMed
- 18. Yeniad B, Beginoglu M, Bilgin LK. Lid-wiper epitheliopathy in contact lens users and patients with dry eye. Eye Contact Lens 2010;36:140‒3. ArticlePubMed
- 19. Gipson IK. Distribution of mucins at the ocular surface. Exp Eye Res 2004;78:379‒88. ArticlePubMed
- 20. Fahmy AM, Hardten DR. Treating ocular surface disease: new agents in development. Clin Ophthalmol 2011;5:465‒72. ArticlePubMedPMC
- 21. Takaoka-Shichijo Y, Sakamoto A, Nakamura M. Effect of diquafosol tetrasodium on MUC5AC secretion by rabbit conjunctival tissues. Eye 2011;28:261‒5.
- 22. Yuko S, Masatsugu N. Stimulatory effect of diquafosol tetrasodium on the expression of membrane-binding mucin genes in cultured human corneal epithelial cells. J Eye 2011;28:425‒9.
- 23. Guthrie SE, Jones L, Blackie CA, Korb DR. A comparative study between an oil-in-water emulsion and nonlipid eye drops used for rewetting contact lenses. Eye Contact Lens 2015;41:373‒7. ArticlePubMed
- 24. Ngo W, Srinivasan S, Houtman D, Jones L. The relief of dry eye signs and symptoms using a combination of lubricants, lid hygiene and ocular nutraceuticals. J Optom 2017;10:26‒33. ArticlePubMedPMC
- 25. Itakura H, Kashima T, Itakura M, et al. Topical rebamipide improves lid wiper epitheliopathy. Clin Ophthalmol 2013;7:2137‒41. ArticlePubMedPMC
- 26. Efron N, Brennan NA, Morgan PB, Wilson T. Lid wiper epitheliopathy. Prog Retin Eye Res 2016;53:140‒74. ArticlePubMed
Citations
Citations to this article as recorded by

 , In Ho Woo
, In Ho Woo 



 KSCRS
KSCRS

 ePub Link
ePub Link Cite
Cite