Articles
- Page Path
- HOME > Insights Cataract Refract Surg > Volume 0; > Article
- Original Article 두 기계에서 회선-직선 복합 방식 초음파유화술과 회선 방식 초음파유화술 비교
-
이지영1, 김은철2

- Comparison of combined torsional and conventional ultrasound mode versus torsional ultrasound mode phacoemulsification in different machines
-
Jiyoung Emily Lee1, Eun Chul Kim2

-
DOI: https://doi.org/10.63375/icrs.25.018
Published online: April 30, 2026
1Department of Ophthalmology, Yeouido St. Mary’s Hospital, College of Medicine, The Catholic University of Korea, Seoul, Korea
2Department of Ophthalmology, Bucheon St. Mary’s Hospital, College of Medicine, The Catholic University of Korea, Seoul, Korea
- 0 Views
- 0 Download
- 0 Crossref
- 0 Scopus
Abstract
Purpose
This study aimed to compare the clinical outcomes of phacoemulsification performed using a combined torsional and conventional ultrasound mode versus torsional ultrasound mode alone in cataract surgery.
Methods
Sixty-five patients who underwent phacoemulsification using combined torsional and conventional ultrasound mode with the Cube alpha system (Nidek Co.) were compared with 300 patients who underwent phacoemulsification using torsional ultrasound mode alone with the Centurion system (Alcon Research Ltd.). The two groups were classified as N3, N4, N5, or N6 according to the Lens Opacities Classification System III. In each subgroup, phacoemulsification time (seconds), cumulative dissipated energy (CDE), balanced salt solution (BSS) use, and postoperative best-corrected visual acuity were analyzed and compared between the combined-mode group and the torsional-only group.
Results
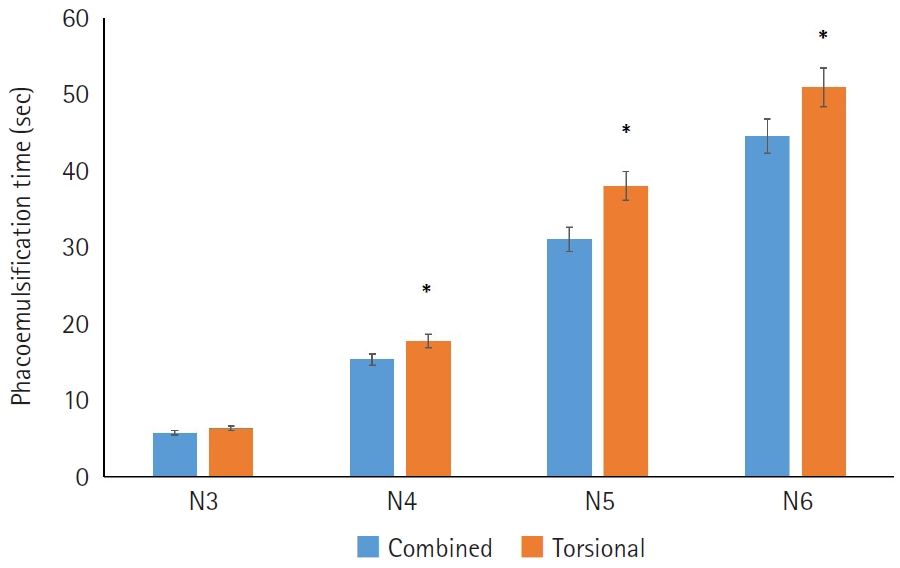
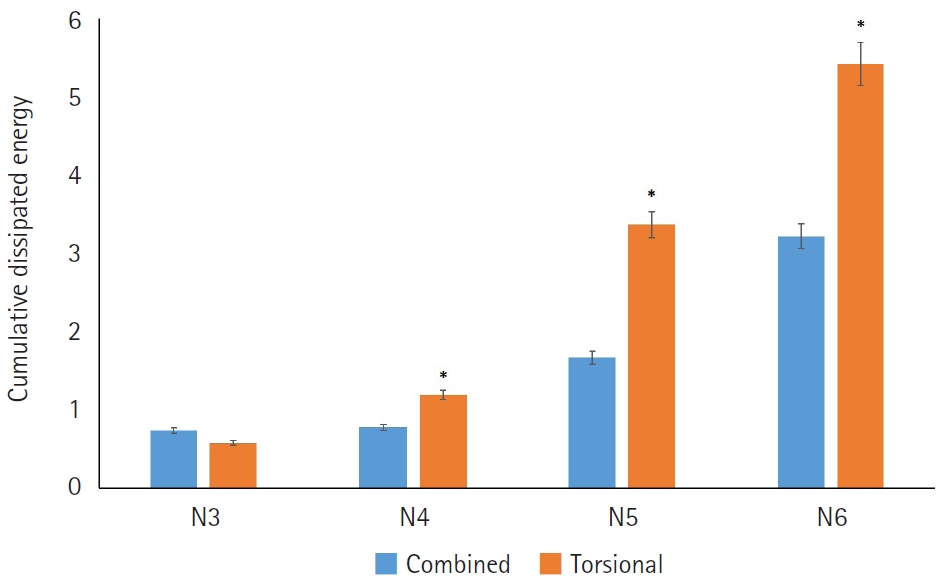
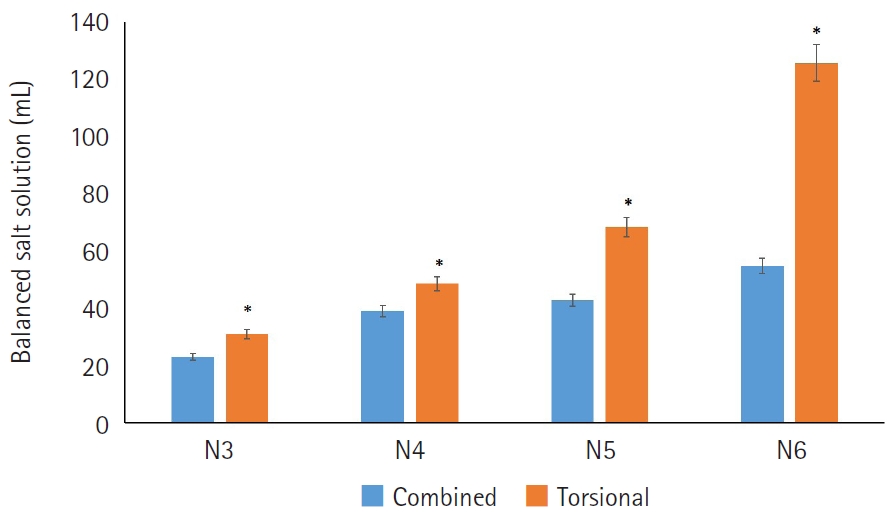
In the N4–N6 subgroups, the torsional-only group had significantly longer phacoemulsification times and higher CDE values than the combined-mode group (P<0.05 for all comparisons). In the N3–N6 subgroups, the total volume of BSS used in the torsional-only group (N3, 30.97±11.05; N4, 48.56±20.06; N5, 68.27±23.06; N6, 125.64±45.67) was significantly greater than that used in the combined-mode group (N3, 23.01±10.27; N4, 39.03±24.16; N5, 42.86±18.24; N6, 54.75±0.75) (P<0.05). There were no statistically significant differences between the groups in postoperative manifest refraction spherical equivalent, corneal endothelial cell loss, or best-corrected visual acuity.
Conclusion
Compared with torsional ultrasound mode alone, the combined torsional and conventional ultrasound mode was more efficient in terms of ultrasound time, CDE, and BSS use. This advantage was more evident with increasing nuclear sclerosis grade.
- Figure

 KSCRS
KSCRS

 Cite
Cite