-
Results of multifocal intraocular lens implantation in patients who underwent corneal refractive surgery
-
Eun Chul Kim
-
Insights Cataract Refract Surg 2025;10(3):76-82. Published online October 31, 2025
-
DOI: https://doi.org/10.63375/icrs.25.011
-
-
 Abstract Abstract
 PDF PDF ePub ePub
- Purpose
The aim of this study was to evaluate the clinical results of multifocal intraocular lenses in patients who underwent corneal refractive surgery.
Methods
Thirty eyes (16 patients; Synergy: ZFR00V) were retrospectively enrolled. Uncorrected and corrected near visual acuity (UNVA, CNVA), intermediate visual acuity (UIVA, CIVA), and distant visual acuity (UDVA, CDVA), manifest refraction spherical equivalent (MRSE), and satisfaction score were assessed before and after surgery.
Results
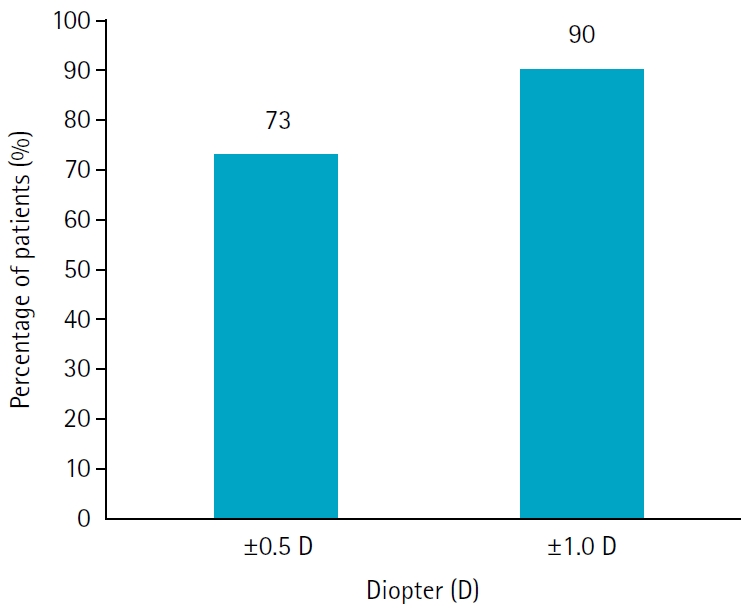
The postoperative UDVA, UIVA, UNVA, and MRSE of the three groups exhibited improvements compared to the preoperative data (P<0.05). The error between the postoperative refraction and the intraocular lens calculation was smaller with the Barrett True K formula than with the Haigis-L formula (P<0.05). The defocus curve at 0 diopter (D) increased, from –1 to –1.5 D, and from –2.5 to –4.0 D, indicating improved vision at distant, intermediate, and near distances. Distance satisfaction (1.47±0.63), near satisfaction (1.25±0.71), and overall satisfaction (1.36±0.42) were good, but light scattering and halo satisfaction (1.97±0.85) yielded a poor result.
Conclusion
In patients with cataracts who underwent corneal refractive surgery, multifocal intraocular lens implantation resulted in excellent uncorrected visual acuity at distant, intermediate, and near distances. However, careful consideration should be given to patient selection due to the incidence of side effects such as glare and halos.
-
Efficacy of extended depth of focus, enhanced monofocal, and monofocal intraocular lenses in patients with retinal disease
-
Eun Chul Kim
-
Insights Cataract Refract Surg 2025;10(2):52-60. Published online June 30, 2025
-
DOI: https://doi.org/10.63375/icrs.25.009
-
-
 Abstract Abstract
 PDF PDF ePub ePub
- Purpose
The aim of this study was to compare the visual quality of extended depth of focus (EDOF), enhanced monofocal, and monofocal intraocular lenses (IOLs) in patients with retinal disease.
Methods
In total, 103 eyes from 93 patients (group 1: enhanced monofocal ICB00, n=36; group 2: EDOF ZXR00, n=36; group 3: monofocal ZCB00, n=31) were retrospectively enrolled. Uncorrected and corrected near visual acuity (UNVA, CNVA), intermediate visual acuity (UIVA, CIVA), and distance visual acuity (UDVA, CDVA), manifest refraction spherical equivalent (MRSE), and satisfaction scores were assessed before and after surgery.
Results
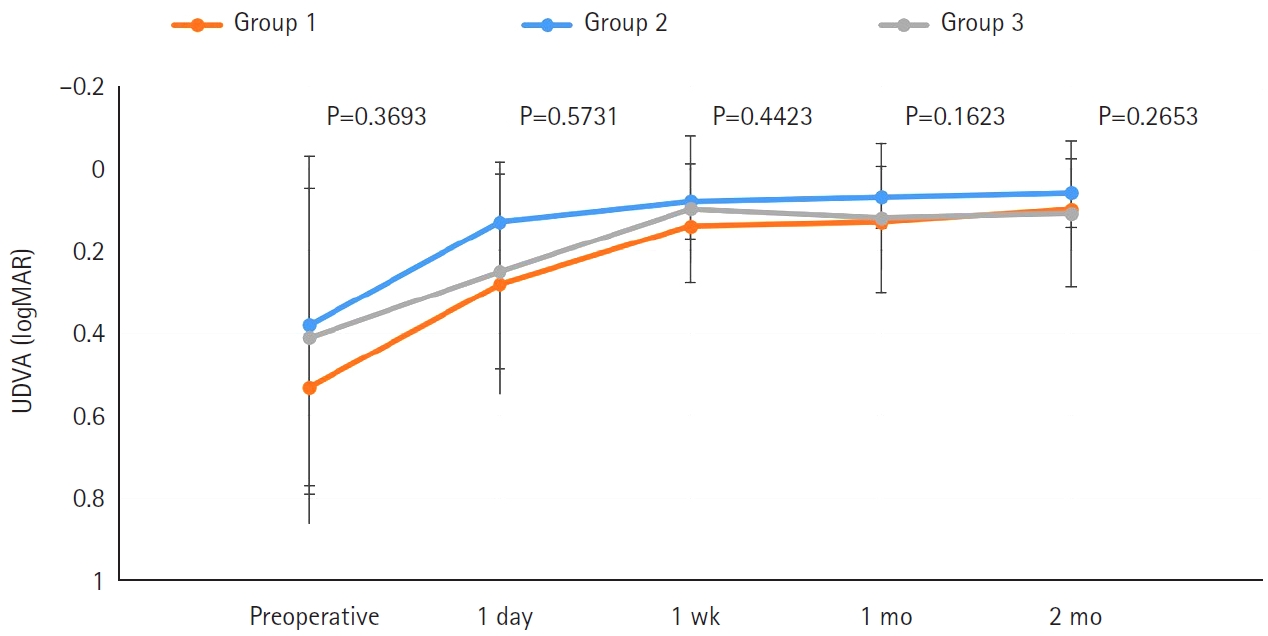
The postoperative UDVA, CDVA, and MRSE of the three groups were better than the preoperative data, respectively (P<0.05). The UIVA of group 1 (0.13±0.12 logMAR) and 2 (0.10±0.11) was significantly better than that of groups 3 (0.25±0.15) (P<0.05). The UNVA of group 2 (0.18±0.12) was significantly better than that of groups 1 (0.32±0.20) and 3 (0.45±0.26; P<0.05). The UDVA of patients with macular edema and macular holes was insignificantly lower than that of epiretinal membranes and high myopia. The overall satisfaction of group 1 (1.58±0.81) and 2 (1.46±0.75) was significantly better than that of groups 3 (1.83±0.97; P<0.05).
Conclusion
EDOF and enhanced monofocal IOLs were associated with better intermediate and near vision than monofocal IOLs in patients with retinal disease. However, monofocal IOLs are recommended in patients with macular edema and macular holes, unlike patients with epiretinal membranes and high myopia.
-
Comparison of combined torsional and conventional ultrasound mode versus torsional ultrasound mode phacoemulsification in different machines
-
Jiyoung Emily Lee, Eun Chul Kim
-
Received December 28, 2025 Accepted April 7, 2026 Published online April 30, 2026
-
DOI: https://doi.org/10.63375/icrs.25.018
-
-
 Abstract Abstract
 ePub ePub
- Purpose
This study aimed to compare the clinical outcomes of phacoemulsification performed using a combined torsional and conventional ultrasound mode versus torsional ultrasound mode alone in cataract surgery.
Methods
Sixty-five patients who underwent phacoemulsification using combined torsional and conventional ultrasound mode with the Cube alpha system (Nidek Co.) were compared with 300 patients who underwent phacoemulsification using torsional ultrasound mode alone with the Centurion system (Alcon Research Ltd.). The two groups were classified as N3, N4, N5, or N6 according to the Lens Opacities Classification System III. In each subgroup, phacoemulsification time (seconds), cumulative dissipated energy (CDE), balanced salt solution (BSS) use, and postoperative best-corrected visual acuity were analyzed and compared between the combined-mode group and the torsional-only group.
Results
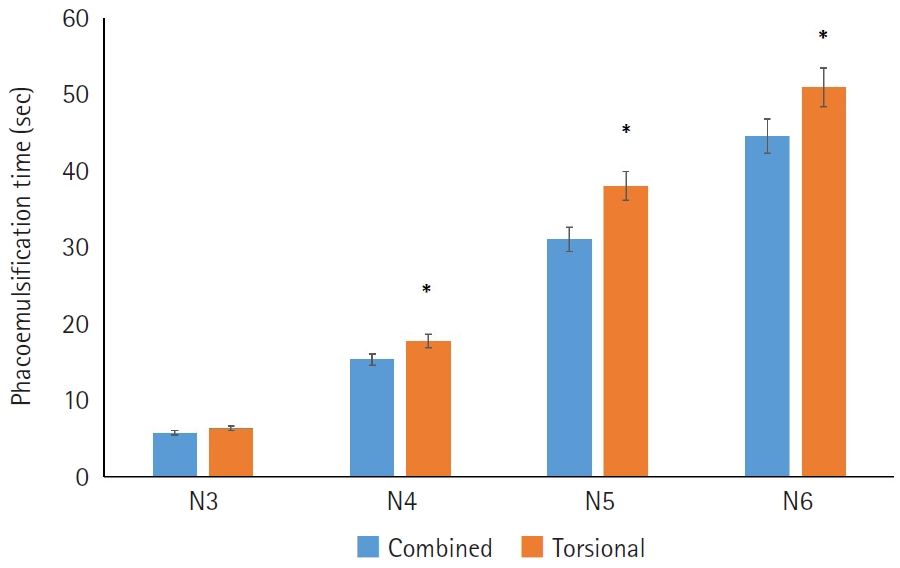
In the N4–N6 subgroups, the torsional-only group had significantly longer phacoemulsification times and higher CDE values than the combined-mode group (P<0.05 for all comparisons). In the N3–N6 subgroups, the total volume of BSS used in the torsional-only group (N3, 30.97±11.05; N4, 48.56±20.06; N5, 68.27±23.06; N6, 125.64±45.67) was significantly greater than that used in the combined-mode group (N3, 23.01±10.27; N4, 39.03±24.16; N5, 42.86±18.24; N6, 54.75±0.75) (P<0.05). There were no statistically significant differences between the groups in postoperative manifest refraction spherical equivalent, corneal endothelial cell loss, or best-corrected visual acuity.
Conclusion
Compared with torsional ultrasound mode alone, the combined torsional and conventional ultrasound mode was more efficient in terms of ultrasound time, CDE, and BSS use. This advantage was more evident with increasing nuclear sclerosis grade.
|